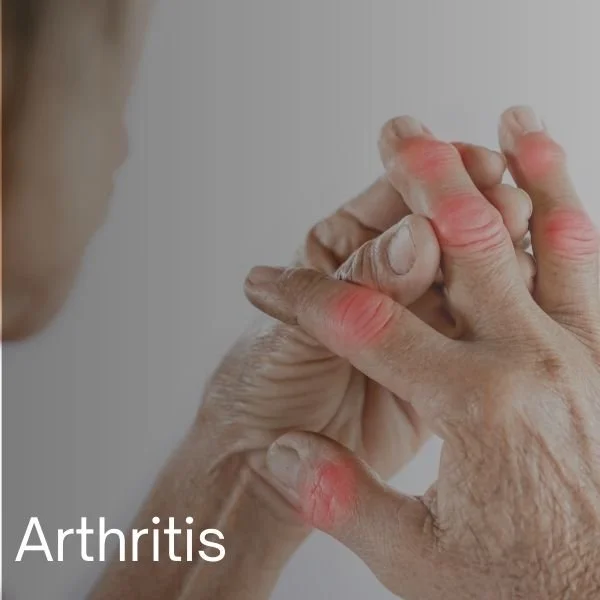
Your pain is real.
So is the relief.
Stanford's Dr. David Spiegel has spent 50 years researching how the mind changes what the body feels.
In a single 10-minute session, 77% of Reveri users felt less pain. No drugs. No side effects.
77% of users felt less pain after a single 10-minute session

Clinically proven
Most users notice a meaningful shift in their first session

Relief in minutes
Guided by Dr. Spiegel
His voice leads every session - interactive, responsive, personal

As seen in



When pain won't let you live your life.
You’ve probably tried things that helped a little. Or worked for a week, then stopped. Chronic pain is exhausting - not just physically, but in every way. Reveri works differently: instead of blocking pain signals from the outside, Dr. Spiegel guides your mind to change how it processes them from within.
77% of our users feel less pain.
In one session. With no drugs.
Grounded in 50+ years of research by Stanford's Dr. David Spiegel.

David Spiegel, M.D.
Associate Chair of Psychiatry


4.6/5 (5,000+ reviews)
Real People, Real Relief
How Reveri helps with chronic pain.
Most pain treatments work from the outside: they block signals, reduce inflammation, or numb sensation. Reveri works differently. Dr. Spiegel guides you into a state of highly focused concentration - and in that state, your mind can directly change how your body experiences pain. Studies show hypnosis can reduce pain by 30–42%. In Reveri's own user data, 77% of users felt less pain after a single session. No drugs. No side effects. Safe for daily use.
Common questions about hypnosis for pain
-
Yes, and the evidence is substantial. Studies show hypnosis can reduce pain intensity by 30-42%. In Reveri's own data, 77% of users reported meaningful pain reduction after a single 10-minute session. Self-hypnosis works by guiding the mind into a state of highly focused attention in which it can directly alter how the body processes pain signals, without drugs, without side effects.
-
Hypnosis is not a replacement for prescribed medication, but research supports its use as a complementary or standalone tool for pain management. Unlike medication, hypnosis has no side effects, no risk of dependency, and can be used daily. It works through a different mechanism: rather than blocking pain chemically, it changes how the brain processes and perceives pain.
-
77% of Reveri users felt less pain after a single 10-minute session. Most people notice a shift before the session ends. The effect can deepen with regular use, but meaningful relief in the first session is common, not the exception.

You've tried other things. Try this.
10 minutes. No drugs. No side effects. 7-day free trial. Most people know after the first session whether it works for them.
Self-hypnosis App for pain: Pain management hypnotherapy
Diagnosis or not, hypnosis can help individuals achieve pain relief. Chronic (lasting longer than 3-6 months) and acute (short-lived) conditions, such as the following, can benefit from hypnosis for pain management.
FAQ
-
Yes, and the evidence is not new. Clinical research on hypnosis for chronic pain goes back decades. In a single 10-minute Reveri session, 77% of users felt less pain. Dr. Spiegel guides you into a state of highly focused attention, and in that state your mind can directly change how your body experiences pain. No drugs. No side effects. Safe for daily use.
-
The strongest evidence is for chronic pain, where hypnosis has been studied most deeply and where effect sizes are largest. Research also supports its use for stress, sleep disruption, and habit change. Reveri delivers sessions across all of these, guided by Dr. Spiegel's 50+ years of research.
-
Yes. In one 10-minute Reveri session, 77% of users felt less pain. In that state of highly focused attention, your mind can directly influence how your body processes pain signals, reducing both the sensation and the emotional weight of it. Studies show hypnosis can reduce pain by 30-42%. It’s safe for daily use. No drugs, no side effects.
-
Early research suggests a link between hypnosis and reduced inflammatory markers, but this area is still being studied. The evidence for pain reduction itself is much stronger, and that is what Reveri's sessions are built around.
-
Because it works, and because it's one of the few approaches that carries no side effects, no risk of dependency, and no drug interactions. Hypnosis has been used in clinical settings for decades. Dr. Spiegel has published more than 400 research papers on it. In Reveri, that same approach is available in 10-minute sessions, whenever you need one.
-
That's exactly how Reveri was designed to work. Each session is 10 minutes, guided by Dr. Spiegel's voice, and available whenever you need it, in bed, at work, on a flight. The state of focused attention you enter during a session is the same state his patients enter in his clinic.
Research: Understanding Hypnosis and
Its Effects on Pain
Can hypnosis help with pain relief?
Let’s begin with the conclusion: hypnosis is scientifically proven to be one of the best drug-free ways to reduce pain. [1] Importantly, hypnosis reduces many different types of clinical pain that people deal with in their lives, both acute and chronic. [2] But before we explain how hypnosis is so effective for reducing pain, let’s review what pain is and how the brain manages painful experiences.
-
Pain is a universal form of suffering. While most of us will have to deal with acute (or sharp) pain at different points in our lives (e.g., injury, surgery), some may face chronic pain for medical and other reasons. Pain is sensed mainly through bare nerve endings; thicker nerve cells send information about pain from an acute injury (like getting a cut), while thinner ones communicate dull pain (like after surgery or long-lasting tissue damage) and temperature. Pain information is sent to different places in the brain. One of these routes sends information to the thalamus (often described as the brain’s “relay station”) and then to the somatosensory cortex (the part of the brain that processes physical sensory information including touch).
Other brain areas beyond the somatosensory cortex become active during pain sensation. Some of these areas include the anterior cingulate cortex (a key structure in the Salience Network which detects threat or novel information), the insula (a brain-body relay also part of the Salience Network), the prefrontal cortex (a key structure in the Executive Control Network), the amygdala (often associated with strong emotions such as fear and anger), and the hippocampus (responsible for forming memories). The amygdala and hippocampus react to the emotional impact of having pain, not the painful sensation itself. Pain is known to have a far-reaching impact on us beyond sensory discomfort, and often evokes strong emotions and memories. Although the context in which the pain is felt matters, pain is mostly associated with unpleasant emotions. In fact, pain and depression often go hand in hand, with chronic pain closely linked to low mood and lack of motivation. On the other hand, people with depression are more pain-sensitive. That’s why some languages use the same word for “in pain” and “depressed.”
How hypnosis helps
Hypnotic suggestions are the content that is delivered using hypnosis to communicate the change we want. As such, hypnotic suggestions that deal with pain could address the sensory component of pain (targeting pain reduction) or the emotional component of pain (targeting how bothersome a painful sensation could be). As discussed in more depth in our article about the Brain’s Activity During Hypnosis, parts of the Salience Network change the way we process information during hypnosis. The same Salience Network also processes pain information and participates in the emotional, cognitive, and behavioral components of experiencing pain [3]. With hypnosis, your brain can reduce the extent to which pain bothers you and help you minimize its effects on your daily life. Hypnosis can also literally reduce the amount of pain you feel. The strain in pain lies mainly in the brain.
When suggestions target pain sensation itself, hypnosis changes the activity of the somatosensory cortex [4]. Hypnosis can reduce pain by almost 30% in most people and up to 42% in those with high hypnotizability [1]. And this finding is encouragingly consistent across the scientific literature: hypnosis results in a greater reduction of clinical pain in more than 70% of individuals when compared to control conditions (when study participants receive a task different from hypnosis) [2].
This means that you can significantly reduce your pain levels simply by following hypnotic suggestions and allowing your brain to change how you feel.
Why is hypnosis a better alternative?
Hypnosis has been used for decades in and outside clinics, hospitals, and surgery rooms. In one famous study, Dr. Spiegel’s team demonstrated how hypnosis could reduce surgical pain and emotional distress after surgery, reduce complications, shorten procedure time (by 17 minutes on average), and even reduce the need for pain medication by up to 40%! [6] Similar effects have been shown in dental treatment, where reduced pain with hypnosis could lead to a higher treatment success rate, reduced need for pain medication, and decreases in discomfort and anxiety levels [7]. Not only that, hypnosis significantly reduces pain even when compared with standard care and is superior to other psychological interventions for a variety of chronic pain conditions [5].
As noted in The American Journal of Medicine [8], “if hypnosis were a drug, it would be standard of care,” and that hypnosis should be used “particularly when it outperforms the current standard of care as measured by safety and efficacy, as in the case of opioids and sedatives.”
Bottom Line
Hypnosis is one of the best drug-free treatments for pain management. Hypnosis can reduce pain sensation, and in addition it can also reduce the distress and negative emotions associated with experiencing it. At a time when there are more than 100,000 drug overdose deaths per year in the United States, two-thirds of them caused by opioids [9], hypnosis is safer than most pharmacological treatments for pain, can reduce the need for such medication, and can be more effective than common pain treatments.
References
Thompson, T. et al. The effectiveness of hypnosis for pain relief: A systematic review and meta-analysis of 85 controlled experimental trials. Neurosci. Biobehav. Rev. 99, 298–310 (2019).
Milling, L. S., Valentine, K. E., LoStimolo, L. M., Nett, A. M. & McCarley, H. S. Hypnosis and the Alleviation of Clinical Pain: A Comprehensive Meta-Analysis. Int. J. Clin. Exp. Hypn. 69, 297–322 (2021).
Del Casale, A. et al. Neural functional correlates of hypnosis and hypnoanalgesia: Role of the cingulate cortex. Am. J. Clin. Hypn. 64, 53–61 (2022).
Casiglia, E. et al. Mechanisms of Hypnotic Analgesia Explained by Functional Magnetic Resonance (fMRI). Int. J. Clin. Exp. Hypn. 68, 1–15 (2020).
Adachi, T., Fujino, H., Nakae, A., Mashimo, T. & Sasaki, J. A Meta-Analysis of Hypnosis for Chronic Pain Problems: A Comparison Between Hypnosis, Standard Care, and Other Psychological Interventions. Int. J. Clin. Exp. Hypn. 62, 1–28 (2014).
Lang, E. V. et al. Adjunctive non-pharmacological analgesia for invasive medical procedures: a randomised trial. The Lancet 355, 1486–1490 (2000).
Dilmahomed, H. & Jovani-Sancho, M. Hypnoanalgesia in Dentistry: A Literature Review. Am. J. Clin. Hypn. 61, 258–275 (2019).
Kittle, J. & Spiegel, D. Hypnosis: The Most Effective Treatment You Have Yet to Prescribe. Am. J. Med. 134, 304–305 (2021).
https://nida.nih.gov/research-topics/trends-statistics/overdose-death-rates, 2022
About the author:
Afik Faerman, Ph.D. is a postdoctoral scholar at Stanford University. He completed his doctoral training in clinical psychology with an emphasis in neuropsychology, and his clinical training at the University of California, San Francisco (UCSF) and Baylor College of Medicine in Houston, TX. Afik’s research centers on identifying key neurocognitive mechanisms in clinical change, focusing on hypnosis, pain, and sleep. His research was supported and acknowledged by the American Psychological Association, the Society for Clinical and Experimental Hypnosis, and the American Society for Clinical Hypnosis.